Table of Contents
- Introduction
- How Common Is Stress?
- How Stress Works in the Body
- Types of Stress
- Stress, Trauma, and Adversity
- Hidden Sources of Stress
- How Stress Affects Body Systems
- Resilience and Neuroplasticity
- Signs That Stress May Be Affecting You
- Lifestyle Medicine Approaches for Managing Stress
- Evidence-Based Therapies for Stress and Anxiety
- George Washington University (GW) Resources
- Additional Educational and Self-Help Resources
Introduction: What Is Stress?

According to the American Psychological Association (APA, 2025), stress is a normal reaction to everyday pressures. It is the body’s built-in alarm system, designed to help us respond to challenges, stay alert, and protect ourselves from harm. Short-term stress can even be beneficial, for instance, by helping us meet deadlines, perform well under pressure, or react quickly in emergencies (think: running away from a tiger or catching a falling object). This kind of adaptive stress (or eustress) can motivate and energize us.
However, stress becomes unhealthy when it is chronic or overwhelming, disrupting sleep, mood, digestion, focus, and overall wellbeing. When the body remains in “high alert” mode for extended periods, stress begins to harm rather than help. For example, chronic stress is linked to inflammation, heart disease, depression, diabetes, immune dysregulation, and cognitive decline (Braun et al., 2016; Mariotti, 2015).
Importantly, stress is not just an emotional state. It’s a whole-body experience involving the brain, hormones, immune system, and gut. Prolonged activation of the “fight-or-flight” response (the sympathetic nervous system) can reduce our capacity for rest, recovery, and healing. This imbalance is known as allostatic overload, which is a key pathway through which stress contributes to chronic disease (Cohen et al., 2007; Lee et al., 2019).
“Resilience is the process and outcome of successfully adapting to difficult or challenging life experiences.”
— American Psychological Association (2025)
How Common Is Stress?
Stress remains one of the most widespread health challenges in the United States.
According to the American Psychological Association’s Stress in America™ reports (2023–2025):
- The average adult continues to rate their stress at 5 out of 10, higher than before the pandemic.
- 27% of adults report that stress regularly interferes with daily functioning.
- Finances, work, and health remain leading causes of stress, while in 2024–2025, national issues such as the economy and politics were also identified as major stressors.
- Younger adults (18–34) and racially and ethnically diverse populations report the greatest impact, with 56% of Black adults indicating that stress interferes with productivity and well-being.
- Nearly 43% of U.S. adults said they felt more anxious in 2024 than the previous year, with stress and sleep disruption cited as top factors (APA, 2025, Psychiatry.org, 2024).
Stress is universal, yet its impact varies by age, background, trauma history, and access to support. Recognizing these differences helps clinicians and communities tailor care that is both culturally responsive and equitable (Baban & Morton, 2022).
How Stress Works
Understanding the Body’s Stress Response
Stress begins deep in the brain. When a person faces a challenge or perceives a threat, the part of the brain called the hypothalamus activates two major biological pathways:
- the sympathetic nervous system (SNS)—commonly known as the “fight, flight, or freeze” response, and
- the hypothalamic–pituitary–adrenal (HPA) axis, which governs the hormonal cascade that manages prolonged stress.
Together, these systems prepare the body to react quickly. The adrenal glands release adrenaline (epinephrine) and cortisol, hormones that increase heart rate, blood pressure, and blood sugar while diverting blood flow away from digestion and toward the muscles and brain. This acute surge enhances alertness and energy to help you respond to immediate demands, a reaction that once protected our ancestors from predators and now helps us meet deadlines or avoid danger.
This short-term activation is adaptive stress, sometimes called eustress. It is part of normal life and can be motivating and even health-promoting when balanced with periods of rest and recovery.
Once the stressful event passes, the parasympathetic nervous system, often described as “rest and digest”, restores equilibrium. It slows heart rate, lowers blood pressure, and signals the body to resume repair processes such as digestion, immune function, and hormone balance.
However, when stress is frequent, intense, or prolonged, these same biological systems remain active for too long. The body’s alarm system no longer shuts off, leading to a constant state of physiological arousal. Elevated cortisol and adrenaline over time disrupt sleep, appetite, and mood regulation, while also promoting inflammation, insulin resistance, and immune suppression (Cohen et al., 2007; Mariotti, 2015).
In this way, the stress response, originally meant to protect, can become damaging when chronically engaged.
Over time, chronic stress can affect:
- The heart and circulation: raising blood pressure and risk for heart disease.
- The brain and mood: increasing anxiety, depression, and memory problems.
- The gut: altering digestion and the gut microbiome.
- The immune system: lowering resistance to infections and slowing recovery.
Types of Stress
Not all stress is harmful. Understanding the different forms helps individuals recognize how the body reacts and when to intervene.
- Acute stress: A short-term response to immediate challenges such as public speaking or narrowly avoiding an accident. This stress is normal and often beneficial, as it promotes focus and performance. (American Psychological Association, 2023; McEwen, 2007)
- Episodic acute stress: Occurs when frequent short-term stressors pile up, like constant deadlines or recurring family conflicts, leading to irritability, muscle tension, or exhaustion. (The American Institute of Stress, 2025; Schneiderman et al., 2005)
- Chronic stress: Continuous stress from ongoing situations such as financial hardship, caregiving, or unsafe living conditions. This is the type most harmful to long-term health. (Cohen et al., 2019; McEwen, 2011)
- Toxic stress: Severe or prolonged stress, especially in childhood, without adequate social or emotional support. This is particularly harmful during childhood as it can disrupt brain development, alter immune and hormonal systems, and increase risk for chronic disease throughout life (Felitti et al., 1998; Shonkoff et al., 2012).
- Harvard University Center on the Developing Child-Toxic Stress
- Harvard University Toxic Stress Resource Guide
Understanding where stress comes from and how it functions allows patients to identify when normal stress has become chronic and needs attention.
Stress, Trauma, and Adversity
Stress does not exist in isolation. For many people, stress is layered across time and experience. Adverse Childhood Experiences (ACEs), such as neglect, violence, or exposure to substance misuse, can heighten the body’s reactivity to stress later in life. ACEs have been associated with over 40 physical and mental health conditions across the lifespan (Wulsin et al., 2022).
Ongoing social adversity in adulthood, such as racism, poverty, or chronic discrimination, also activates the same biological stress pathways. These chronic exposures have been shown to amplify inflammatory signaling and allostatic load, promoting inequities in health outcomes across populations (Shonkoff et al., 2009).
A trauma-informed perspective recognizes that such patterns reflect survival adaptations rather than personal weakness. Healing requires restoring a sense of safety in both the body and one’s environment. Supportive relationships, culturally responsive care, and lifestyle practices that regulate the nervous system, such as mindful breathing, restorative sleep, and physical activity, can help reverse physiological dysregulation (Braun et al., 2016; Lee et al., 2019).
Hidden Sources of Stress

Stress is not always overt. Many forms of modern stress are subtle, cumulative, and environmental. Identifying these hidden sources is an important first step toward change.
- Workplace and financial stress: Long hours, job insecurity, or debt sustain low-level activation of the stress response. Over time, this contributes to burnout and physical illness.
- Health-related stress: Living with chronic pain, sleep disorders, or caregiving responsibilities can drain physical reserves and resilience.
- Social and environmental stress: Loneliness, lack of community, and exposure to unsafe or polluted environments activate the same biological stress systems as physical danger.
- Cultural and racial stress: Repeated experiences of microaggressions, social exclusion, or systemic inequities can create a state of “chronic vigilance,” raising baseline stress hormones (Shonkoff et al., 2009).
Recognizing these less obvious stressors helps individuals set boundaries, seek social support, and make small adjustments, like scheduling rest, connecting with others, or engaging in mindfulness, that restore physiological balance.
How Stress Affects Body Systems
Stress doesn’t just happen “in your head.” It is a whole-body experience linking the brain, gut, heart, hormones, and immune system, which is a dynamic network often referred to as the mind–body connection.
When stress is short-term, the body adapts effectively and then returns to balance. But when stress is frequent or unrelieved, the stress response systems, especially the hypothalamic-pituitary-adrenal (HPA) axis, stay activated. This prolonged activation keeps cortisol and adrenaline levels high, leading to chronic, low-grade inflammation. Over time, this state of “biological wear and tear” is known as allostatic load, which disrupts cellular repair, immune signaling, and metabolic function (McEwen & Seeman, 1999; Mariotti, 2015).
Chronic stress has been linked to numerous conditions, including hypertension, cardiovascular disease, diabetes, depression, and dementia (Cohen et al., 2007; Mariotti, 2015). Understanding how stress interacts with body systems helps explain why lifestyle approaches, like nutrition, movement, sleep, and mindfulness, are so essential for prevention and recovery (Braun et al., 2016; Lee et al., 2019).
The Brain and Nervous System
The brain both triggers and experiences stress. When the HPA axis is repeatedly activated, cortisol affects key brain structures:
- The hippocampus, which supports memory and learning, may shrink under prolonged stress, leading to forgetfulness and difficulty concentrating.
- The amygdala, which processes fear and emotional reactivity, becomes overactive, increasing anxiety and vigilance.
- The prefrontal cortex, responsible for focus and decision-making, becomes less efficient, which can impair judgment and impulse control.
These brain changes explain why chronic stress often leads to irritability, mood swings, or insomnia. Fortunately, interventions such as mindfulness, slow breathing, and relaxation training can retrain neural circuits, enhance emotional regulation, and promote recovery of hippocampal volume and function (Feder et al., 2009; Lee et al., 2019).
The Cardiovascular System
Stress activates the sympathetic nervous system, causing the adrenal glands to release adrenaline and noradrenaline. These hormones raise heart rate and constrict blood vessels, increasing blood pressure to prepare the body for action.
When this response occurs occasionally, it poses no harm. But if sustained, the repeated surges of pressure and inflammation damage blood vessel walls, encourage plaque buildup, and elevate the risk for hypertension, arrhythmias, and atherosclerosis (Mariotti, 2015).
Over time, stress can become as significant a contributor to cardiovascular disease as diet or smoking. Protective strategies, such as daily movement, social connection, deep breathing, and gratitude, help regulate heart rhythm and blood pressure (Braun et al., 2016).
The Endocrine and Metabolic Systems
The HPA axis controls cortisol release from the adrenal glands. Cortisol helps mobilize glucose for energy during acute stress. However, chronic cortisol elevation raises blood sugar and insulin levels, leading to insulin resistance, weight gain, and fatigue.
Prolonged stress also disrupts thyroid hormones, reproductive hormones (such as estrogen and testosterone), and growth hormone, contributing to low libido, menstrual irregularities, and decreased energy. These imbalances can worsen mood disorders and metabolic disease if left unchecked (Mariotti, 2015).
Lifestyle approaches that promote hormone balance, particularly restorative sleep, balanced nutrition, and regular activity, help normalize cortisol rhythms and metabolic health (Lee et al., 2019).
The Immune System
Acute stress can temporarily boost immune readiness, preparing the body to heal and defend. But chronic stress has the opposite effect: it suppresses white blood cell activity, increases inflammation, and slows recovery from illness or injury (Cohen et al., 2007; Mariotti, 2015).
Long-term cortisol elevation alters immune cell gene expression, reducing antiviral defense and increasing vulnerability to colds, infections, and even slower wound healing. Chronic inflammation also contributes to autoimmune activity and has been linked to depression and cardiovascular disease.
Mind–body interventions, social connection, and anti-inflammatory nutrition, rich in plants, fiber, and omega-3 fatty acids, can reduce stress-induced inflammation and strengthen immune balance (Braun et al., 2016; Lee et al., 2019).
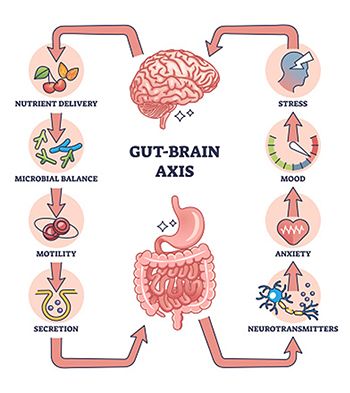
The Gut-Brain Axis
The gut–brain axis describes the two-way communication between your digestive system and central nervous system. Stress disrupts this communication in several ways: it slows digestion, alters gut motility, and changes the composition of gut microbiota.
Chronic stress can also increase intestinal permeability (“leaky gut”), allowing inflammatory molecules to enter the bloodstream and further affect mood and cognition (Cryan et al., 2023; Warren et al., 2024; Warren et al., 2025). These disruptions contribute to symptoms like bloating, indigestion, or irritable bowel syndrome.
Balanced, fiber-rich nutrition, mindful eating, and fermented foods such as yogurt, kimchi, or kefir help restore gut integrity and reduce the gut’s sensitivity to stress (Lee et al., 2019).
The Musculoskeletal System
When the body senses threat, muscles tighten in preparation to protect vital organs. This “brace response” is useful for short-term safety but becomes painful when sustained. Chronic tension in the neck, shoulders, or jaw may cause headaches, back pain, and fatigue.
Simple daily habits, such as stretching, yoga, tai chi, walking, or massage, help relax the musculoskeletal system, restore mobility, and send calming feedback to the brain that the body is safe. This mind-body loop helps downshift the nervous system from fight-or-flight to rest-and-repair mode (Braun et al., 2016).
The Digestive System
Beyond the gut-brain axis, stress directly influences digestive function. During fight-or-flight states, digestion slows as blood flow is redirected to muscles. Chronic stress can suppress appetite for some people or drive emotional eating in others (Warren et al., 2025). Over time, it may contribute to reflux, stomach upset, and nutrient malabsorption.
Mindful eating, taking slow, intentional bites, focusing on the senses, and avoiding distractions, has been shown to support digestion and calm the vagus nerve, the primary pathway of the parasympathetic system that signals rest and safety (Lee et al., 2019; Warren et al., 2024).
The Reproductive System
Persistent stress alters the delicate balance of reproductive hormones. In women, high cortisol can suppress estrogen and progesterone, leading to irregular cycles, infertility, or menopausal symptom flare-ups. In men, chronic stress can reduce testosterone production and sperm quality (Mariotti, 2015).
Healthy sleep, balanced nutrition, and stress-reduction practices can support hormonal regulation and reproductive wellbeing. For those with persistent symptoms, professional evaluation is recommended.
Stress and Body Systems – At A Glance
Stress triggers a cascade of biological changes that influence nearly every organ system. Understanding this helps explain why lifestyle approaches (like movement, nutrition, sleep, and connection) are so effective in restoring balance.
| System | How Stress Affects It | Helpful Lifestyle Approaches |
|---|---|---|
| Musculoskeletal | Muscles tighten as a protective reflex; chronic tension causes pain and headaches. | Gentle stretching, progressive muscle relaxation, yoga. |
| Respiratory | Breathing quickens; may worsen asthma or panic. | Slow, deep breathing, box breathing, guided relaxation. |
| Cardiovascular | Heart rate and blood pressure rise; chronic strain increases risk for heart disease. | Daily movement, relaxation practices, gratitude journaling. |
| Digestive | Alters gut bacteria and slows digestion; may cause nausea or bloating. | Eat slowly, choose fiber-rich and fermented foods. |
| Endocrine | Activates cortisol; chronic elevation contributes to fatigue, insulin resistance, and weight gain. | Prioritize sleep, balanced meals, physical activity. |
| Reproductive | Chronic stress suppresses hormones and libido. | Adequate rest, stress management, medical evaluation if persistent. |
| Immune | Heightened inflammation, increased infection risk. | Nutrition, mindfulness, social connection. |
When stress hormones stay high, inflammation and immune dysfunction follow, raising risk for cardiovascular disease, diabetes, depression, and anxiety (Mariotti, 2015; Vitaliano et al., 2002). The encouraging news: lifestyle medicine interventions, such as physical activity, restorative sleep, whole-food nutrition, and meaningful social connection, can reverse many of these biological effects and strengthen resilience (Lee et al., 2019)
Bringing the Systems Together
Each body system, cardiovascular, endocrine, immune, digestive, musculoskeletal, and neurological, is interconnected through shared stress-response pathways. When cortisol, adrenaline, and inflammation stay elevated, these systems collectively experience allostatic overload.
The good news is that these processes are reversible. Lifestyle medicine interventions—including physical activity, mindful breathing, restorative sleep, social connection, and anti-inflammatory nutrition, can down-regulate stress pathways and restore homeostasis (Braun et al., 2016; Lee et al., 2019). Even small, consistent habits promote healing at the cellular and molecular level.
Key Takeaways
- Stress affects every major body system, not just emotions.
- Chronic activation of the HPA axis leads to allostatic load—long-term “wear and tear.”
- The most vulnerable systems include the cardiovascular, immune, metabolic, and nervous systems.
- Lifestyle medicine tools involving nutrition, movement, sleep, mindfulness, and social connection can reverse stress physiology and build resilience.
- Healing is cumulative: small, daily changes retrain the nervous system and restore balance to the whole body.
Resilience and Neuroplasticity
Resilience refers to the ability to recover and grow from stress. It is not a fixed trait but a dynamic skill that strengthens with practice. Neuroplasticity, the brain’s ability to reorganize and form new connections, underlies this process (Feder et al., 2009).
When individuals practice calming behaviors, like mindfulness, gratitude, exercise, or nurturing relationships, their brain circuits for safety and self-regulation become stronger. These changes occur in the prefrontal cortex (which governs attention and decision-making) and in stress-related areas such as the amygdala and hippocampus, where balanced activity supports emotional control and memory.
Resilience-building practices align with lifestyle medicine principles:
- Mindfulness and meditation reduce HPA axis reactivity and lower cortisol (Lee et al., 2019).
- Physical activity promotes neurogenesis and endorphin release.
- Nutrition and restorative sleep regulate inflammation and circadian rhythms.
- Social connection stimulates oxytocin, a hormone that counteracts stress responses.
Resilience does not eliminate difficulty; it transforms how the body and mind recover from it. Over time, these adaptive pathways can replace stress-driven patterns with healthier, more flexible responses.
Key Takeaways
- Stress is a normal human response, but chronic, unrelieved stress can harm your body and mind.
- Awareness of your own stress patterns is the first step toward change.
- Lifestyle habits such as regular movement, restorative sleep, balanced nutrition, and mindfulness help regulate your stress response.
- Resilience can be learned at any age through consistent practice and support.
- Compassion for yourself is as important as any tool. Healing starts with self-understanding.

Signs That Stress May Be Affecting You
Everyone experiences stress differently. Becoming aware of how it shows up in your body and behavior is the first step toward change. If results suggest high stress or persistent anxiety, reach out to your clinician or a behavioral-health professional for personalized support.
You may notice stress in:
- Body: fatigue, headaches, muscle tension, stomach upset, frequent colds
- Mood: anxiety, irritability, low motivation, sadness
- Behavior: changes in appetite, difficulty concentrating, poor sleep, social withdrawal, increased use of alcohol or nicotine
Try a Quick Self-Check
These brief, validated tools can help you understand how stress is affecting you.
PHQ-4: Ultra-Brief Anxiety & Depression Screening
Over the last 2 weeks, how often have you been bothered by the following problems?
(Circle one option per item)
|
# |
Item |
Not at all (0) |
Several days (1) |
More than half the days (2) |
Nearly every day (3) |
| 1 | Feeling nervous, anxious, or on edge | 0 | 1 | 2 | 3 |
| 2 | Not being able to stop or control worrying | 0 | 1 | 2 | 3 |
| 3 | Little interest or pleasure in doing things | 0 | 1 | 2 | 3 |
| 4 | Feeling down, depressed, or hopeless | 0 | 1 | 2 | 3 |
Scoring
PHQ-4 total score ranges from 0 to 12, with categories of psychological distress being:
- None 0-2
- Mild 3-5
- Moderate 6-8
- Severe 9-12
Kroenke, K., Spitzer, R. L., Williams, J. B., & Löwe, B. (2009). An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics, 50(6), 613–621. https://doi.org/10.1176/appi.psy.50.6.613
Tracking Stress Levels Over Time
The Perceived Stress Scale (PSS-10) is one of the most widely used and validated tools for understanding how stressed you feel in the last month. Tracking your score over time can help you notice patterns, see improvements, and understand which habits make the biggest difference.
Use the PSS-10 here (free):
- PDF version (original):
https://www.das.nh.gov/wellness/docs/percieved%20stress%20scale.pdf - Online scoring tool (patient-friendly):
https://www.mdapp.co/perceived-stress-scale-pss-calculator-389/ - NIH commentary on stress and coping (context):
https://www.nimh.nih.gov/health/publications/stress
Tip: Repeat the PSS-10 every 2–4 weeks to track your stress trends.
Other Validated Tools
- PHQ-2
- PHQ-9 for depression screening
- GAD-7 Anxiety Scale
- Holmes and Rahe Stress Scale (life events)
Lifestyle Medicine Approaches for Managing Stress
Lifestyle Medicine focuses on daily habits that build resilience. Each pillar of lifestyle medicine influences the others. Addressing them together creates the strongest foundation for wellbeing. Small, consistent steps in multiple areas often lead to the most lasting change.
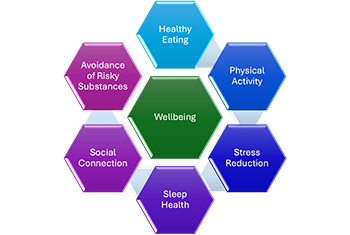
1. Mind-Body and Stress-Reduction Practices

Techniques such as mindfulness, yoga, breathing exercises, and guided imagery retrain the nervous system to shift from “fight-or-flight” to “rest-and-repair.” These tools strengthen the parasympathetic nervous system, the body’s calming branch of the nervous system, and increase heart-rate variability, a key marker of resilience (Pascoe et al., 2017).
Evidence-based tools include:
- Mindfulness-Based Stress Reduction (MBSR): The classic eight-week program shown to lower anxiety, depression, blood pressure, and chronic pain (Khoury et al., 2015).
- Diaphragmatic or “box” breathing: Inhale through the nose for four counts, hold for four, exhale for four, and pause for four. This simple rhythm lowers heart rate and cortisol, and activates the relaxation response.
- Grounding practices: Focus on sensations, sights, or sounds around you to stay present, which can be useful during moments of overwhelm or trauma triggers.
- Gratitude journaling and compassion practices: Shifting attention to appreciation builds positive emotion and social connection.
- Guided imagery and progressive muscle relaxation: Helpful for sleep, anxiety, and chronic pain.
- Spending time in nature or with animals: Nature exposure reduces cortisol, blood pressure, and rumination, while pet interaction releases oxytocin, a bonding hormone (Jimenez et al., 2021).
- Creative flow and play: Activities like music, dance, art, or gardening stimulate “flow states” that reset the nervous system and restore a sense of joy.
Try this: The World Health Organization’s Doing What Matters in Times of Stress is a stress management guide for coping with adversity. The guide aims to equip people with practical skills to help cope with stress. A few minutes each day are enough to practice the self-help techniques. The guide can be used alone or with the accompanying audio exercises.
Informed by evidence and extensive field testing, the guide is for anyone who experiences stress, wherever they live and whatever their circumstances.
Clinical research: Mindfulness and slow breathing can reduce blood pressure and cortisol within weeks (Pascoe et al., 2017; Khoury et al., 2015).
SMART goals for stress reduction:
Choose one practice and make it Specific, Measurable, Achievable, Relevant, and Time-bound. For example: “I’ll take three mindful breaths before checking my phone each morning for one week.”
----ACLM Stress/SMART goal handout-----
----ACLM Take Time for Self-Care handout----
Heart Rate Variability (HRV): A Helpful Window Into Your Stress Levels
Heart rate variability (HRV) is a simple, noninvasive way to understand how your body handles stress. HRV measures the tiny changes in time between each heartbeat. When HRV is higher, it usually means your nervous system is flexible, calm, and able to adapt to challenges. When HRV is low, it can be a sign that your body is under stress and your “fight-or-flight” system is working harder than usual (Kim et al., 2018).
Research shows that both emotional stress and physical strain can lower HRV, and that changes often show up even before you’re aware of feeling stressed (Kim et al., 2018). Because of this, HRV is increasingly used as a helpful marker to understand overall stress load and to track progress when people make lifestyle changes that support better wellbeing.
How HRV Can Support Your Health
While HRV isn’t a diagnostic test, it can give helpful insights into how your body responds to daily stress. Tracking HRV over time can help you:
- See how stress, sleep, and lifestyle habits affect your body
- Notice patterns that may relate to burnout, anxiety, or physical strain
- Monitor how your body responds to relaxation or breathing practices
- Stay motivated by seeing measurable improvements with stress-reduction tools
Many wearables and apps can show your daily HRV trends, helping you understand what helps your body recover and what may be draining your system.
Tools and Practices That Can Improve HRV
Improving HRV is possible—and many science-supported practices can help restore balance to your nervous system.
- HeartMath® Biofeedback
HeartMath® devices (such as Inner Balance® and emWave®) use real-time feedback to guide breathing exercises that improve emotional balance and HRV.
Learn more: https://www.heartmath.org
- Breathing Practices
Breathing slowly at about 5–6 breaths per minute can improve HRV within minutes by activating the calming parasympathetic system (Jerath et al., 2015).
Free resources include:
NIH “Breath Awareness” guide
- Mindfulness & Meditation
Mindfulness practices, such as Mindfulness-Based Stress Reduction (MBSR), are shown to increase HRV by reducing the body’s stress response and improving emotional regulation (Khoury et al., 2013).
MBSR programs: https://www.umassmed.edu/cfm
- Yoga and Tai Chi
Mind-body practices like yoga and tai chi gently activate the parasympathetic nervous system and are associated with increases in HRV and reductions in inflammation (Pascoe et al., 2017).- Tai Chi for Health Institute (Beginner routines):
https://taichiforhealthinstitute.org - NCCIH overview of yoga and tai chi:
https://www.nccih.nih.gov/health - Harvard Health Tai Chi Resources:
https://pll.harvard.edu/course/introduction-tai-chi
https://www.health.harvard.edu/staying-healthy/the-health-benefits-of-tai-chi - Tai Chi Health:
https://taichihealth.com/
- Tai Chi for Health Institute (Beginner routines):
- Healthy Lifestyle Habits
Several everyday habits support higher HRV and better stress resilience, including:- Regular physical activity
- High-quality sleep
- Spending time in nature (Jimenez et al., 2021)
- Meaningful social connection
These behaviors have documented effects on HRV and overall wellbeing (Pascoe et al., 2017).
Bottom Line
HRV is a powerful but easy-to-track way to understand how stress affects your body. With simple daily practices—breathing, mindfulness, movement, and connection—you can support a healthier, more resilient nervous system.
2. Nutrition for Nervous System Resilience

The foods you eat profoundly influence how your body responds to stress. A healthy gut supports a healthy mind through the gut-brain axis, the communication network between intestinal bacteria and brain chemistry (Cryan et al., 2019; Marano et al., 2023). A nutrient-poor diet, such as one high in ultra-processed foods, has been associated with several mental health disorders, as well digestive, neurological, cardiovascular, and autoimmune disorders (Warren et al., 2024; Warren et al., 2025).
Eat more of:
- Leafy greens, berries, and citrus—rich in antioxidants that reduce oxidative stress.
- Fatty fish or flaxseed—omega-3s lower inflammation and stabilize mood.
- Whole grains, legumes, nuts, and seeds—steady blood sugar and sustain energy.
- Fermented foods such as yogurt, kefir, and kimchi—support gut bacteria that produce calming neurotransmitters like GABA and serotonin.
Limit:
- Caffeine and energy drinks, which spike adrenaline.
- Alcohol, which disrupts sleep and mood regulation.
- Ultra-processed or high-sugar foods, which increase inflammation and energy crashes, and can disrupt mood regulation.
Evidence: Diets rich in fruits, vegetables, and omega-3 fatty acids reduce perceived stress and depressive symptoms (Lassale et al., 2019). Emerging studies show fermented foods can reduce anxiety and inflammatory markers (Cryan et al., 2019; Marano et al., 2023).

Tips for mindful eating:
- Eat slowly, without distractions.
- Notice texture, aroma, and taste.
- Pause halfway through meals to check your hunger and fullness cues.
These small shifts activate the parasympathetic system and improve digestion and satisfaction.
- Harvard School of Public Health – Nutrition & Mental Health
https://nutritionsource.hsph.harvard.edu/
https://nutritionsource.hsph.harvard.edu/healthy-eating-plate/
- Harvard: Stress, Health, and Eating Patterns
https://nutritionsource.hsph.harvard.edu/stress-and-health/ - American Heart Association – Healthy Eating Basics
https://www.heart.org/en/healthy-living/healthy-eating - Mediterranean Diet Info (Mayo Clinic)
https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/mediterranean-diet/art-20047801
3. Movement for Mood and Energy

Exercise is one of the most powerful natural stress relievers. It boosts endorphins, improves circulation, and regulates stress hormones. Regular movement literally “re-tunes” the brain’s stress circuits, improving mood, sleep quality (Stubbs et al., 2017), and stress resilience (Nowacka-Chmielewska et al., 2022)
Aim for:
- 150 minutes per week of moderate-intensity activity (brisk walking, cycling, or dancing).
- Strength or resistance training twice weekly.
- Mind-body exercises—yoga, tai chi, or qigong—for flexibility and relaxation.
Movement breaks matter: Even short “movement snacks” (AKA “exercise snacks”), such as a 5-minute stretch or 10-minute walk, can reset your body’s stress response and sharpen focus. You can also include shorter “exercise snacks” of one minute or less of vigorous exercise periodically throughout the day to improve cardiorespiratory fitness (Islam et al., 2022).
Evidence: Regular physical activity is associated with lower anxiety, improved mood, and higher resilience to life stressors (Rebar et al., 2015; Stubbs et al., 2017).
Trauma-informed note: For those with a history of trauma or chronic pain, gentle, choice-based movement (yoga therapy, tai chi, qi gong, walking outdoors, swimming) can restore safety in the body and rebuild confidence.
- Exercise Guidelines – American Heart Association
https://www.heart.org/en/healthy-living/fitness - American Heart Association – Working out to relieve stress
https://www.heart.org/en/healthy-living/healthy-lifestyle/stress-management/working-out-to-relieve-stress - American Psychological Association – Exercise: A healthy stress reliever
https://www.apa.org/news/press/releases/stress/2013/exercise
4. Sleep as a Stress-Recovery Tool
Sleep is the body’s most potent recovery system. During deep sleep, the brain clears waste products, the immune system repairs tissue, and stress hormones reset to baseline (Palagini et al., 2016; Reddy & Van Der Werf, 2020). Yet chronic stress often disrupts this process, and poor sleep, in turn, increases stress reactivity (Direksunthorn, 2025). Further, conditions such as post-traumatic stress disorder (PTSD) frequently involve insomnia and other sleep disturbances from hyperarousal and distressing nightmares (Lancel et al., 2021). A form of cognitive behavioral therapy for insomnia (CBT-I) can target the root cause(s) of insomnia to help improve sleep quality (Lancel et al., 2021)
Tips for better sleep:
- Keep a consistent bedtime and wake time—even on weekends.
- Avoid screens, caffeine, and heavy meals 1–2 hours before bed.
- Try gentle stretching, journaling, or slow breathing to unwind.
- Keep your bedroom cool, dark, and quiet.
- If you snore heavily or have persistent insomnia, speak with your clinician. Conditions such as sleep apnea are common and treatable.
Evidence: Improving sleep hygiene improve mental health (Scott et al., 2021). Even modest improvements in sleep quality can improve cardiometabolic health, such as weight control, blood pressure regulation, and glycemic regulation (Direksunthorn, 2025)
Journaling idea: Before bed, write down three things that went well or one thing you’re grateful for. Gratitude practices shift focus from worry to calm and have been linked to lower inflammatory markers (Komase et al., 2021).
- CDC Sleep Hygiene Guide:
https://www.cdc.gov/sleep - AASM Sleep Education:
https://sleepeducation.org - NIH “Healthy Sleep” Tips:
https://www.nhlbi.nih.gov/health/sleep - GW Lifestyle Medicine Sleep Resources:
https://gwdocs.com/specialties/lifestyle-medicine/sleep
4. Connection, Purpose, and Meaning

Humans are wired for connection. Social relationships are among the strongest predictors of wellbeing, more powerful than exercise or diet alone (Holt-Lunstad, 2022). Supportive connection buffers the effects of stress and fosters resilience across the lifespan.
Ways to strengthen connection:
- Schedule regular contact with friends, family, or coworkers.
- Join group activities, volunteer programs, or faith communities.
- Explore creative or spiritual practices that bring meaning.
- Practice kindness and gratitude—both lower cortisol and boost immune function (Komase et al., 2021).
Evidence: Social connection improves cardiovascular, immune, and mental-health outcomes (Martina et al., 2015; Holt-Lunstad, 2022). Conversely, loneliness and isolation increase mortality risk comparable to smoking (Office of the Surgeon General, 2023).
Equity and inclusion note: Experiences of discrimination or exclusion can magnify stress. Finding culturally affirming spaces, such as community groups, spiritual organizations, or peer networks, can restore belonging and safety.
Connection is medicine. Meaning gives stress a purpose.
- NIH: Social Wellness
https://www.nih.gov/health-information/social-wellness-toolkit - Greater Good Science Center – Purpose & gratitude practices:
https://ggsc.berkeley.edu/
6. Substance Use and Stress
Psychoactive drugs directly affect your stress response (Sinha, 2024). Substances such as alcohol, nicotine, and cannabis may seem to “take the edge off,” but they often worsen stress in the long run by harming HPA-axis regulation and disrupting sleep, mood, and hormonal balance (Sinha, 2008; Sinha, 2024).
If you rely on these substances to cope:
- Reach out for support—effective help is available and confidential.
- Ask your clinician about evidence-based cessation programs or medications.
Resources:
- SAMHSA National Helpline: 1-800-662-4357 (24/7, free, confidential)
- Quitline for Tobacco: 1-800-QUIT-NOW
Evidence: Substance use as a coping mechanism increases long-term anxiety and cortisol sensitivity (Sinha, 2008). Recovery efforts not only improve mental clarity but also enhance physical health and resilience.
Create Your Personalized Stress Action Plan
Start small—choose one strategy per category (mind-body, nutrition, movement, sleep, connection) and track how you feel after one week.
You can use a “My Stress Dashboard” or Mood Tracker to note energy, mood, and sleep patterns. Reflection builds self-awareness and motivation.
Reflection prompt: “When do I feel most calm, connected, or energized—and what small action helped me get there?”
Over time, these micro-habits compound into powerful health changes.
When to Seek Professional Support

Everyone experiences stress, but when it becomes persistent, overwhelming, or interferes with daily functioning, professional support can be an important step toward recovery and resilience. The American Psychological Association (2023), the CDC (2023), and the National Institute of Mental Health (2023) all recommend seeking help when stress leads to prolonged sadness or anxiety, sleep disruption, withdrawal, physical symptoms, or thoughts of hopelessness. Reaching out to a healthcare or mental-health provider is a proactive and effective way to regain balance and build long-term coping skills.
Signs It’s Time to Reach Out
Consider connecting with a healthcare or mental-health professional if stress is:
- Causing persistent sadness, panic, irritability, or fatigue
- Interfering with sleep, work, or relationships
- Leading to withdrawal, increased substance use, or loss of interest in daily activities
- Triggering physical symptoms such as headaches, chest pain, or digestive problems
- Accompanied by thoughts of hopelessness or self-harm
If you’re unsure whether what you’re feeling “counts” as stress or anxiety, talking with a clinician, even briefly, can help you find clarity and options for care.
Resources:
- GW Lifestyle Medicine: Avoidance of Harmful Substances Resources
https://gwdocs.com/specialties/lifestyle-medicine/avoidance-harmful-substances
Evidence-Based Therapies for Stress and Anxiety
Effective, research-supported therapies can reduce stress, strengthen resilience, and improve overall wellbeing:
- Cognitive Behavioral Therapy (CBT): Focuses on identifying and reframing unhelpful thought patterns that fuel stress or anxiety. CBT helps you practice new, evidence-based coping strategies to change both mindset and behavior to manage stress (Nakao et al., 2021).
- Acceptance and Commitment Therapy (ACT): Encourages mindfulness, cognitive flexibility, and values-based living, teaching you to accept what’s outside your control while committing to actions that reflect your deepest priorities (Anusuya & Gayatridevi, 2025)
- Mindfulness-Based Stress Reduction (MBSR): Combines meditation, yoga, and self-awareness to calm the body’s stress response and increase compassion for oneself and others. Studies show MBSR can reduce anxiety, pain, and blood pressure (Khoury et al., 2015).
Find evidence-based providers near you at FindTreatment.gov.
George Washington University (GW) Resources
If you’re part of the GW community or local DC area, confidential, affordable counseling and therapy services are available:
- GW Center Clinic — A community mental-health clinic offering low-cost, sliding-scale counseling provided by supervised doctoral students in clinical psychology.
psyd.columbian.gwu.edu/clinic | (202) 994-4929
- GW Community Counseling Services Center (CCSC) — Provides individual, couple, and family counseling in a supportive environment.
gsehd.gwu.edu/ccsc | (202) 994-8645
- GW Resiliency and Wellbeing Center - The R&W Center takes an evidence-based, whole person approach in the health and wellness (well-being) services it provides to the GW medical enterprise—SMHS, GW MFA, and the GW Hospital. The R&W Center provides individual-, departmental-, and institutional-level services.
https://rwc.smhs.gwu.edu/
Crisis Support
If you ever feel unsafe with your thoughts or worry you might harm yourself, immediate help is available:
- Call or text 988 or chat 988lifeline.org — Suicide and Crisis Lifeline (24/7, free, confidential)
- If in danger or needing urgent care, go to your nearest emergency department or call 911.
- Veterans and service members can press “1” after dialing 988 for specialized support.
You are not alone—help works, and recovery is always possible.
Additional Educational and Self-Help Resources
These trusted organizations provide evidence-based information, guided tools, and self-care practices for managing stress:
- American Psychological Association - Stress
- American Psychological Association – Stress Effects on the Body
- World Health Organization – Stress
- World Health Organization-Doing What Matters in Times of Stress Audio Guide
- World Health Organization – Self-Help Plus Program
- Centers for Disease Control and Prevention – Stress
- Centers for Disease Control and Prevention – Managing Stress
- National Institutes of Health – Your Healthiest Self: Wellness Toolkits
- Harvard Health Online – Stress
- Harvard Health Online – Understanding the Stress Response
Common Apps for Stress Management
References
A Guide to Toxic Stress and Early Childhood Development. (2005, May 14). Center on the Developing Child at Harvard University. https://developingchild.harvard.edu/resource-guides/guide-toxic-stress/
Abe, M., & Abe, H. (2019). Lifestyle medicine – An evidence based approach to nutrition, sleep, physical activity, and stress management on health and chronic illness. Personalized Medicine Universe, 8, 3–9. https://doi.org/10.1016/j.pmu.2019.05.002
American Adults Express Increasing Anxiousness in Annual Poll; Stress and Sleep are Key Factors Imp. (n.d.). Retrieved November 12, 2025, from https://www.psychiatry.org:443/news-room/news-releases/annual-poll-adults-express-increasing-anxiousness
Baban, K. A., & Morton, D. P. (2022). Lifestyle Medicine and Stress Management. The Journal of Family Practice, 71((1 Suppl Lifestyle)). https://doi.org/10.12788/jfp.0285
Braun, C., Foreyt, J. P., & Johnston, C. A. (2016a). Stress: A Core Lifestyle Issue. American Journal of Lifestyle Medicine, 10(4), 235–238. https://doi.org/10.1177/1559827616642400
Braun, C., Foreyt, J. P., & Johnston, C. A. (2016b). Stress: A Core Lifestyle Issue. American Journal of Lifestyle Medicine, 10(4), 235–238. https://doi.org/10.1177/1559827616642400
CDC. (2025a, June 10). Managing Stress. Mental Health. https://www.cdc.gov/mental-health/living-with/index.html
CDC. (2025b, June 10). Managing Stress. Mental Health. https://www.cdc.gov/mental-health/living-with/index.html
Cohen, S., Janicki-Deverts, D., & Miller, G. E. (2007). Psychological Stress and Disease. JAMA, 298(14), 1685. https://doi.org/10.1001/jama.298.14.1685
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A Global Measure of Perceived Stress. Journal of Health and Social Behavior, 24(4), 385. https://doi.org/10.2307/2136404
Cohen, S., Murphy, M. L. M., & Prather, A. A. (2019). Ten Surprising Facts About Stressful Life Events and Disease Risk. Annual Review of Psychology, 70(1), 577–597. https://doi.org/10.1146/annurev-psych-010418-102857
Crielaard, L., Nicolaou, M., Sawyer, A., Quax, R., & Stronks, K. (2021). Understanding the impact of exposure to adverse socioeconomic conditions on chronic stress from a complexity science perspective. BMC Medicine, 19(1), 242. https://doi.org/10.1186/s12916-021-02106-1
Cryan, J. F., O’Riordan, K. J., Cowan, C. S. M., Sandhu, K. V., Bastiaanssen, T. F. S., Boehme, M., Codagnone, M. G., Cussotto, S., Fulling, C., Golubeva, A. V., Guzzetta, K. E., Jaggar, M., Long-Smith, C. M., Lyte, J. M., Martin, J. A., Molinero-Perez, A., Moloney, G., Morelli, E., Morillas, E., … Dinan, T. G. (2019). The Microbiota-Gut-Brain Axis. Physiological Reviews, 99(4), 1877–2013. https://doi.org/10.1152/physrev.00018.2018
Diniz, G., Korkes, L., Tristão, L. S., Pelegrini, R., Bellodi, P. L., & Bernardo, W. M. (2023). The effects of gratitude interventions: a systematic review and meta-analysis. Einstein (Sao Paulo, Brazil), 21, eRW0371. https://doi.org/10.31744/einstein_journal/2023RW0371
Direksunthorn, T. (2025). Sleep and Cardiometabolic Health: A Narrative Review of Epidemiological Evidence, Mechanisms, and Interventions. International Journal of General Medicine, Volume 18, 5831–5843. https://doi.org/10.2147/IJGM.S563616
Feder, A., Nestler, E. J., & Charney, D. S. (2009). Psychobiology and molecular genetics of resilience. Nature Reviews Neuroscience, 10(6), 446–457. https://doi.org/10.1038/nrn2649
Felitti, V. J., Anda, R. F., Nordenberg, D., Williamson, D. F., Spitz, A. M., Edwards, V., Koss, M. P., & Marks, J. S. (1998). Relationship of Childhood Abuse and Household Dysfunction to Many of the Leading Causes of Death in Adults. American Journal of Preventive Medicine, 14(4), 245–258. https://doi.org/10.1016/S0749-3797(98)00017-8
Help for Mental Illnesses—National Institute of Mental Health (NIMH). (n.d.). Retrieved November 16, 2025, from https://www.nimh.nih.gov/health/find-help
Hofmann, S. G., Asnaani, A., Vonk, I. J. J., Sawyer, A. T., & Fang, A. (2012). The Efficacy of Cognitive Behavioral Therapy: A Review of Meta-analyses. Cognitive Therapy and Research, 36(5), 427–440. https://doi.org/10.1007/s10608-012-9476-1
Holmes And Rahe Stress Scale Calculator. (n.d.). MDApp. Retrieved November 16, 2025, from https://www.mdapp.co/holmes-and-rahe-stress-scale-calculator-253/
Holmes, T. H., & Rahe, R. H. (1967). The social readjustment rating scale. Journal of Psychosomatic Research, 11(2), 213–218. https://doi.org/10.1016/0022-3999(67)90010-4
Holt-Lunstad, J. (2022). Social Connection as a Public Health Issue: The Evidence and a Systemic Framework for Prioritizing the “Social” in Social Determinants of Health. Annual Review of Public Health, 43(1), 193–213. https://doi.org/10.1146/annurev-publhealth-052020-110732
Identifying and relieving stress. (2024, August 13). Harvard Health. https://www.health.harvard.edu/topics/stress
Islam, H., Gibala, M. J., & Little, J. P. (2022). Exercise Snacks: A Novel Strategy to Improve Cardiometabolic Health. Exercise and Sport Sciences Reviews, 50(1), 31–37. https://doi.org/10.1249/JES.0000000000000275
Jerath, R., Crawford, M. W., Barnes, V. A., & Harden, K. (2015). Self-Regulation of Breathing as a Primary Treatment for Anxiety. Applied Psychophysiology and Biofeedback, 40(2), 107–115. https://doi.org/10.1007/s10484-015-9279-8
Jimenez, M. P., DeVille, N. V., Elliott, E. G., Schiff, J. E., Wilt, G. E., Hart, J. E., & James, P. (2021). Associations between Nature Exposure and Health: A Review of the Evidence. International Journal of Environmental Research and Public Health, 18(9), 4790. https://doi.org/10.3390/ijerph18094790
John, N. A., John, J., Tarnikanti, M., Kalpana, M., Kamble, P., Singhal, A., Ganji, V., Gaur, A., Umesh, M., Katta, R., Saktivadivel, V., Daulatabad, V. S., Singaravelu, V., & Vamishidhar, I. S. (2023). Implications of lifestyle medicine in medical practice. Journal of Family Medicine and Primary Care, 12(2), 208–212. https://doi.org/10.4103/jfmpc.jfmpc_1587_22
Khoury, B., Lecomte, T., Fortin, G., Masse, M., Therien, P., Bouchard, V., Chapleau, M.-A., Paquin, K., & Hofmann, S. G. (2013). Mindfulness-based therapy: A comprehensive meta-analysis. Clinical Psychology Review, 33(6), 763–771. https://doi.org/10.1016/j.cpr.2013.05.005
Kim, H. G., Cheon, E. J., Bai, D. S., Lee, Y. H., & Koo, B. H. (2018). Stress and Heart Rate Variability: A Meta-Analysis and Review of the Literature. Psychiatry investigation, 15(3), 235–245. https://doi.org/10.30773/pi.2017.08.17
Komase, Y., Watanabe, K., Hori, D., Nozawa, K., Hidaka, Y., Iida, M., Imamura, K., & Kawakami, N. (2021). Effects of gratitude intervention on mental health and well-being among workers: A systematic review. Journal of Occupational Health, 63(1), e12290. https://doi.org/10.1002/1348-9585.12290
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2003). The Patient Health Questionnaire-2: Validity of a Two-Item Depression Screener. Medical Care, 41(11), 1284–1292. https://doi.org/10.1097/01.MLR.0000093487.78664.3C
Kroenke, K., Spitzer, R. L., Williams, J. B. W., & Lowe, B. (2009). An Ultra-Brief Screening Scale for Anxiety and Depression: The PHQ-4. Psychosomatics, 50(6), 613–621. https://doi.org/10.1176/appi.psy.50.6.613
Lancel, M., Van Marle, H. J. F., Van Veen, M. M., & Van Schagen, A. M. (2021). Disturbed Sleep in PTSD: Thinking Beyond Nightmares. Frontiers in Psychiatry, 12, 767760. https://doi.org/10.3389/fpsyt.2021.767760
Lassale, C., Batty, G. D., Baghdadli, A., Jacka, F., Sánchez-Villegas, A., Kivimäki, M., & Akbaraly, T. (2019a). Healthy dietary indices and risk of depressive outcomes: A systematic review and meta-analysis of observational studies. Molecular Psychiatry, 24(7), 965–986. https://doi.org/10.1038/s41380-018-0237-8
Lassale, C., Batty, G. D., Baghdadli, A., Jacka, F., Sánchez-Villegas, A., Kivimäki, M., & Akbaraly, T. (2019b). Healthy dietary indices and risk of depressive outcomes: A systematic review and meta-analysis of observational studies. Molecular Psychiatry, 24(7), 965–986. https://doi.org/10.1038/s41380-018-0237-8
Lee, J., Papa, F., Jaini, P. A., Alpini, S., & Kenny, T. (2020). An Epigenetics-Based, Lifestyle Medicine–Driven Approach to Stress Management for Primary Patient Care: Implications for Medical Education. American Journal of Lifestyle Medicine, 14(3), 294–303. https://doi.org/10.1177/1559827619847436
Lippman, D., Stump, M., Veazey, E., Guimarães, S. T., Rosenfeld, R., Kelly, J. H., Ornish, D., & Katz, D. L. (2024). Foundations of Lifestyle Medicine and its Evolution. Mayo Clinic Proceedings: Innovations, Quality & Outcomes, 8(1), 97–111. https://doi.org/10.1016/j.mayocpiqo.2023.11.004
Marano, G., Mazza, M., Lisci, F. M., Ciliberto, M., Traversi, G., Kotzalidis, G. D., De Berardis, D., Laterza, L., Sani, G., Gasbarrini, A., & Gaetani, E. (2023). The Microbiota–Gut–Brain Axis: Psychoneuroimmunological Insights. Nutrients, 15(6), 1496. https://doi.org/10.3390/nu15061496
Mariotti, A. (2015). The Effects of Chronic Stress On Health: New Insights Into the Molecular Mechanisms of Brain–Body Communication. Future Science OA, 1(3), FSO23. https://doi.org/10.4155/fso.15.21
Maslach, C., & Jackson, S. E. (1981). The measurement of experienced burnout. Journal of Organizational Behavior, 2(2), 99–113. https://doi.org/10.1002/job.4030020205
McEwen, B. S. (2007). Physiology and Neurobiology of Stress and Adaptation: Central Role of the Brain. Physiological Reviews, 87(3), 873–904. https://doi.org/10.1152/physrev.00041.2006
McEwen, B. S., & Gianaros, P. J. (2011). Stress- and Allostasis-Induced Brain Plasticity. Annual Review of Medicine, 62(1), 431–445. https://doi.org/10.1146/annurev-med-052209-100430
McEWEN, B. S., & Seeman, T. (1999). Protective and Damaging Effects of Mediators of Stress: Elaborating and Testing the Concepts of Allostasis and Allostatic Load. Annals of the New York Academy of Sciences, 896(1), 30–47. https://doi.org/10.1111/j.1749-6632.1999.tb08103.x
Nakao, M., Shirotsuki, K., & Sugaya, N. (2021). Cognitive–behavioral therapy for management of mental health and stress-related disorders: Recent advances in techniques and technologies. BioPsychoSocial Medicine, 15(1), 16. https://doi.org/10.1186/s13030-021-00219-w
Nowacka-Chmielewska, M., Grabowska, K., Grabowski, M., Meybohm, P., Burek, M., & Małecki, A. (2022). Running from Stress: Neurobiological Mechanisms of Exercise-Induced Stress Resilience. International Journal of Molecular Sciences, 23(21), 13348. https://doi.org/10.3390/ijms232113348
Office of the Surgeon General (OSG). (2023). Our Epidemic of Loneliness and Isolation: The U.S. Surgeon General’s Advisory on the Healing Effects of Social Connection and Community. US Department of Health and Human Services. http://www.ncbi.nlm.nih.gov/books/NBK595227/
P, A. S., & S, G. (2025). Acceptance and Commitment Therapy and Psychological Well-Being: A Narrative Review. Cureus. https://doi.org/10.7759/cureus.77705
Palagini, L., Bruno, R. M., Paolo, T., Caccavale, L., Gronchi, A., Mauri, M., Riemann, D., & Drake, C. L. (2016). Association Between Stress-Related Sleep Reactivity and Metacognitive Beliefs About Sleep in Insomnia Disorder: Preliminary Results. Behavioral Sleep Medicine, 14(6), 636–649. https://doi.org/10.1080/15402002.2015.1065406
Pascoe, M. C., Thompson, D. R., & Ski, C. F. (2017). Yoga, mindfulness-based stress reduction and stress-related physiological measures: A meta-analysis. Psychoneuroendocrinology, 86, 152–168. https://doi.org/10.1016/j.psyneuen.2017.08.008
Ravi, M., Miller, A. H., & Michopoulos, V. (2021). The immunology of stress and the impact of inflammation on the brain and behaviour. BJPsych Advances, 27(3), 158–165. https://doi.org/10.1192/bja.2020.82
Read, 1 Min. (n.d.). Stress effects on the body. Https://Www.Apa.Org. Retrieved November 12, 2025, from https://www.apa.org/topics/stress/body
Rebar, A. L., Stanton, R., Geard, D., Short, C., Duncan, M. J., & Vandelanotte, C. (2015). A meta-meta-analysis of the effect of physical activity on depression and anxiety in non-clinical adult populations. Health Psychology Review, 9(3), 366–378. https://doi.org/10.1080/17437199.2015.1022901
Reddy, O. C., & Van Der Werf, Y. D. (2020). The Sleeping Brain: Harnessing the Power of the Glymphatic System through Lifestyle Choices. Brain Sciences, 10(11), 868. https://doi.org/10.3390/brainsci10110868
Resilience. (n.d.). Https://Www.Apa.Org. Retrieved November 12, 2025, from https://www.apa.org/topics/resilience
Schneiderman, N., Ironson, G., & Siegel, S. D. (2005). Stress and Health: Psychological, Behavioral, and Biological Determinants. Annual Review of Clinical Psychology, 1(1), 607–628. https://doi.org/10.1146/annurev.clinpsy.1.102803.144141
Scott, A. J., Webb, T. L., Martyn-St James, M., Rowse, G., & Weich, S. (2021). Improving sleep quality leads to better mental health: A meta-analysis of randomised controlled trials. Sleep Medicine Reviews, 60, 101556. https://doi.org/10.1016/j.smrv.2021.101556
SELF-HELP PLUS (SH+). (n.d.). Retrieved November 12, 2025, from https://www.who.int/publications/i/item/9789240035119
Shonkoff, J. P., Boyce, W. T., & McEwen, B. S. (2009). Neuroscience, Molecular Biology, and the Childhood Roots of Health Disparities: Building a New Framework for Health Promotion and Disease Prevention. JAMA, 301(21), 2252. https://doi.org/10.1001/jama.2009.754
Shonkoff, J. P., Garner, A. S., THE COMMITTEE ON PSYCHOSOCIAL ASPECTS OF CHILD AND FAMILY HEALTH, COMMITTEE ON EARLY CHILDHOOD, ADOPTION, AND DEPENDENT CARE, AND SECTION ON DEVELOPMENTAL AND BEHAVIORAL PEDIATRICS, Siegel, B. S., Dobbins, M. I., Earls, M. F., Garner, A. S., McGuinn, L., Pascoe, J., & Wood, D. L. (2012). The Lifelong Effects of Early Childhood Adversity and Toxic Stress. Pediatrics, 129(1), e232–e246. https://doi.org/10.1542/peds.2011-2663
Sinha, R. (2008). Chronic Stress, Drug Use, and Vulnerability to Addiction. Annals of the New York Academy of Sciences, 1141(1), 105–130. https://doi.org/10.1196/annals.1441.030
Sinha, R. (2024). Stress and substance use disorders: Risk, relapse, and treatment outcomes. Journal of Clinical Investigation, 134(16), e172883. https://doi.org/10.1172/JCI172883
Slavich, G. M. (2020). Social Safety Theory: A Biologically Based Evolutionary Perspective on Life Stress, Health, and Behavior. Annual Review of Clinical Psychology, 16(1), 265–295. https://doi.org/10.1146/annurev-clinpsy-032816-045159
Spitzer, R. L. (1999). Validation and Utility of a Self-report Version of PRIME-MDThe PHQ Primary Care Study. JAMA, 282(18), 1737. https://doi.org/10.1001/jama.282.18.1737
Spitzer, R. L., Kroenke, K., Williams, J. B. W., & Löwe, B. (2006). A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Archives of Internal Medicine, 166(10), 1092. https://doi.org/10.1001/archinte.166.10.1092
Stress. (n.d.-a). Https://Www.Apa.Org. Retrieved November 12, 2025, from https://www.apa.org/topics/stress
Stress. (n.d.-b). Retrieved November 12, 2025, from https://www.who.int/news-room/questions-and-answers/item/stress
Stress | How Right Now | Centers for Disease Control and Prevention. (2024, April 10). https://www.cdc.gov/howrightnow/emotion/stress/index.html
Stress in America. (n.d.). Https://Www.Apa.Org. Retrieved November 12, 2025, from https://www.apa.org/pubs/reports/stress-in-america
Stubbs, B., Vancampfort, D., Rosenbaum, S., Firth, J., Cosco, T., Veronese, N., Salum, G. A., & Schuch, F. B. (2017). An examination of the anxiolytic effects of exercise for people with anxiety and stress-related disorders: A meta-analysis. Psychiatry Research, 249, 102–108. https://doi.org/10.1016/j.psychres.2016.12.020
Toolbox. (n.d.). UCSF SMN. Retrieved November 15, 2025, from https://www.stressmeasurement.org/measurement-toolbox
Toxic Stress: What is toxic stress? (2005, May 14). Center on the Developing Child at Harvard University. https://developingchild.harvard.edu/key-concept/toxic-stress/
Understanding the stress response. (2011, June 15). Harvard Health. https://www.health.harvard.edu/staying-healthy/understanding-the-stress-response
Vitaliano, P. P., Zhang, J., & Scanlan, J. M. (2003). Is Caregiving Hazardous to One’s Physical Health? A Meta-Analysis. Psychological Bulletin, 129(6), 946–972. https://doi.org/10.1037/0033-2909.129.6.946
Warren, A., & Frame, L. A. (2025). Restoring a Healthy Relationship with Food by Decoupling Stress and Eating: A Translational Review of Nutrition and Mental Health. Nutrients, 17(15), 2466. https://doi.org/10.3390/nu17152466
Warren, A., Nyavor, Y., Beguelin, A., & Frame, L. A. (2024). Dangers of the chronic stress response in the context of the microbiota-gut-immune-brain axis and mental health: A narrative review. Frontiers in Immunology, 15, 1365871. https://doi.org/10.3389/fimmu.2024.1365871
WHAT IS STRESS? (n.d.). The American Institute of Stress. Retrieved November 16, 2025, from https://www.stress.org/what-is-stress/
Wulsin, L. R., Sagui-Henson, S. J., Roos, L. G., Wang, D., Jenkins, B., Cohen, B. E., Shah, A. J., & Slavich, G. M. (2022). Stress Measurement in Primary Care: Conceptual Issues, Barriers, Resources, and Recommendations for Study. Psychosomatic Medicine, 84(3), 267–275. https://doi.org/10.1097/PSY.0000000000001051
Yaribeygi, H., Panahi, Y., Sahraei, H., Johnston, T. P., & Sahebkar, A. (2017). The impact of stress on body function: A review. EXCLI Journal; 16:Doc1057; ISSN 1611-2156. https://doi.org/10.17179/EXCLI2017-480
Your Healthiest Self: Wellness Toolkits | National Institutes of Health (NIH). (2025, January 21). https://www.nih.gov/health-information/your-healthiest-self-wellness-toolkits
